
Dr. Dilip Raja
Urologist & Andrologist
Best Doctor for Prostate cancer in Mumbai | Leading Urologist Andrologist – Dr. Dilip Raja
Dr.Dilip Raja ,a renowned Urologist & Andrologist, leading prostate cancer specialist in Mumbai specialized in treating Prostate cancer and other urological disease with more than 35 years of Experience using Advanced Techniques such as Radiation therapy, Hormone treatment & Minimally invasive procedures, Ensuring Optimal Patients outcomes with faster recovery.
Early Detection is a Key!
Consult Urologist today for expert Diagnosis and personalized Treatment with Best Doctor for Prostate Cancer in Mumbai
Get in touch with us today +91 9820074649
Prostate adenocarcinoma, Carcinoma of prostate, Cancer of prostate, Adenocarcinoma of prostate, Prostate carcinoma, Prostate malignancy, Prostate Tumour.
The prostate is a walnut-sized gland that forms part of the male reproductive system. It consists of two lobes or regions enclosed by an outer layer of tissue. It lies in front of the rectum and just below the urinary bladder, which stores urine. The prostate gland surrounds the urethra, the canal through which urine exits the body.
The size of the gland varies with age. In adult men, a typical prostate measures about 3 cm thick and 4 cm wide and weighs about 20 grams. As age advances, the prostate gland increases in size and can range from 40 grams to 100 grams or more.
Prostate cancer ranks among the top ten leading cancers in India today. It usually affects men aged 50 years and above. However, reports increasingly show cases in younger men aged 35–44 and 55–64, especially in metropolitan cities.
Prostate cancer, like any other cancer, develops when abnormal cells grow and divide, forming a tumour.
Prostate cancer tends to become more virulent or aggressive when it occurs in younger individuals. In contrast, it often grows more slowly in older men; therefore, regular prostate screening becomes important after the age of 50
Dr Dilip Raja Provides advanced Diagnosis and treatments plans for both early and advanced stage. As the best doctor for prostate cancer in Mumbai , He has 35+ years of experience in diagnosing and treating prostate cancer with high success rate .
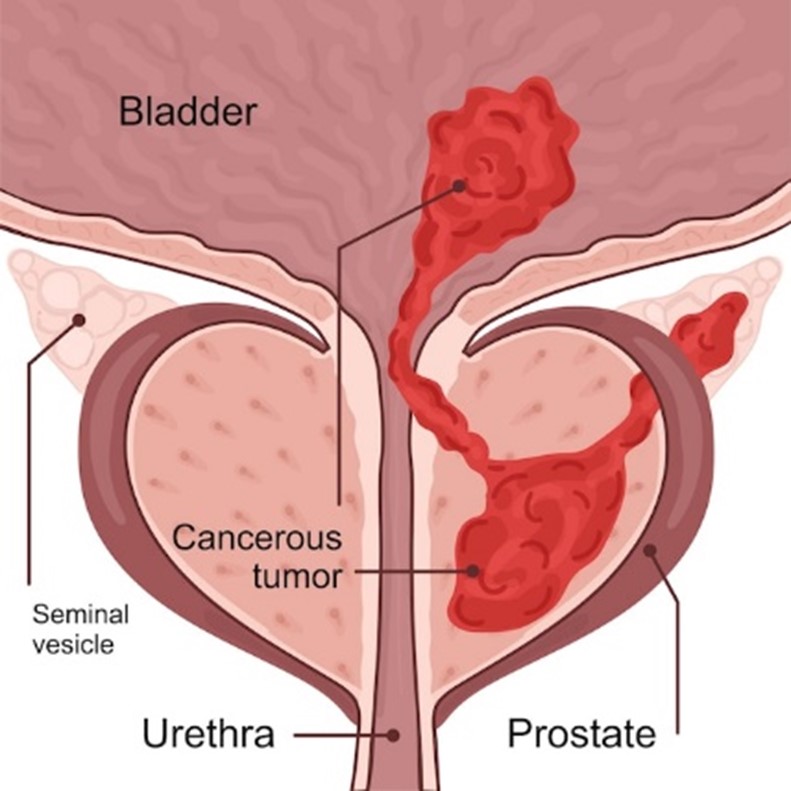
Causes Of Prostate cancer
- Old age
- Obesity
- Improper diet
- Genetic alterations have been identified as some of the main contributing factors towards an increased cause of prostate cancer
Risk Factors
There are four well-established risk factors for prostate cancer:
Men have a 1 in 6 lifetime risk of developing prostate cancer. It accounts to around 10000 deaths.
- Increasing age: -the older men get, the more likely a cancer might develop in the prostate.
- Ethnic origin: -Afro-Caribbean men are at higher risk than Caucasians and men from the Far East have a lower risk for cancer.
- Family history (genetic/heredity): – Risk is increased if a father, brother or paternal uncle has prostate cancer.
- Obesity -Recent studies have shown that men who are over weight are at significantly higher risk for developing prostate cancer.
However, there are some other factors which may impact risk of developing prostate cancer, which are not well understood.
However, early diagnosis and treatment could result in cure as early treatment of clinically significant prostate cancer has a very high cure rate.
Symptoms Of Prostate cancer
- Difficulty urinating,
- Hesitancy,
- Frequent urination
- Sense of incomplete voiding
- Taking a long time to pass urine
- Blood in the urine (haematuria).
These symptoms may or may not be present in early stage of prostate cancer. Hence, the regular screening is required. If the Prostate Cancer is detected and treated early the survival chances greatly increase. Please contact immediately your health provider best Urologist, Andrologist & Uro-Oncologist Dr. Dilip Raja Mumbai, India for complete treatment of prostate cancer.
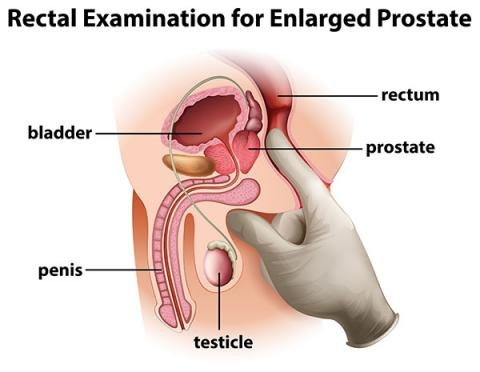
Physical Examinitation For Prostate cancer
The digital rectal exam (DRE)
Digital Rectal Examination by an experienced urologist is a must to differentiate between benign and cancerous prostate. A healthy prostate feels soft, rubbery, smooth, symmetrical, regular and even. Any lumps, or hard, woody or irregular areas of the prostate may indicate the presence of cancer and will require further testing.

Normal BPH
Tenderness

Symmetrical Enlarged

Asymmetrical
Induction

Nodularity
Investigations
- PSA TEST
- USG ABDOMEN & PELVIS WITH FULL BLADDER & POST VOID RESIDUAL URINE
- TRANSRECTAL ULTRASONOGRAPHY (TRUS) OF THE PROSTATE
- MRI OF PELVIS
- TRUS GUIDED PROSTATE NEEDLE BIOPSY
- BONE SCAN
- PET CT SCAN OR PSMA PET SCAN
- X-RAY CHEST PA VIEW
The PSA test

The PSA, or prostate-specific antigen test, is the most common prostate cancer test. This simple blood test measures the level of prostate-specific antigen (PSA) circulating in the bloodstream. It usually serves as the first step in diagnosing prostate cancer. In addition, the PSA test tracks the effects of prostate cancer treatment such as surgery, radiation, hormone therapy, and chemotherapy.
Readings -Cancer detection
PSA levels
- Normal – 0 TO 4 ng/dl
- Borderline – 4 – 10 ng/dl
- Significant –more than 10 ng/dl
Once DRE and PSA are suspicious of prostate cancer, the next step is to do USG of abdomen and pelvis with post void residual urine subsequently, MRI of the prostate before doing Prostate Biopsy.
USG For Abdomen & Pelvis With Full Bladder And Post Void Residual Urine Combined With Transrectal Ultrasonography (TRUS) Of The Prostate
- The urinary system and also measure the status of both kidneys.
- Bladder Capacity and Post Void Residual Urine.
- Approximate size of the Prostate Gland.
MRI of The Pelvis (Magnetic Resonance Imaging)
MRI of the pelvis will not only detect the irregularity of prostate but also give an idea of local extension of the prostate cancer, if present & it will also give us a clue of the prostate spreading outside capsule of the prostate or into the lymph nodes.
Guided Prostate Biopsy
Clinicians perform TRUS-guided prostate needle biopsy under local anaesthesia in a sonography unit. During this procedure, they use transrectal ultrasound guidance and obtain 12–16 cores of prostatic tissue by inserting a needle through the rectum. After that, they send the tissue samples for histopathological examination.
Bone Scan
When a tumour damages a bone, new bone tissue forms. A bone scan detects this new growth and can show whether the cancer has spread into the bone. This scan helps check for the spread of cancer to the bone.
PET CT Scan Or PSMA PET Scan
PSMA PET scan is an imaging test that detects prostate cancer throughout the body. It uses a radioactive substance that targets a protein called PSMA (Prostate-Specific Membrane Antigen), which prostate cancer expresses.
X RAY CHEST PA VIEW
Grading of Prostate cancer
- The pathologist grade cancer cell removed during biopsies
- Low grade looks more like normal cells
- High grade, cell may vary in size and shape
- Cell from two biopsy site is graded using Gleason score of between 2 –10. The higher the score, the more likely cancer cells will grow faster and spread. The pathologist will give your doctor a report about biopsy.
Gleason’s Score
The Gleason’s score not only keeps grades the disease but also predict the prognosis of prostate cancer.
| Score 0 – 6 | Score of 7 | Score up to 8 – 10 |
| The cancer can be a slow-growing tumour; therefore, clinicians often take a conservative approach. If the cancer is small and localized, they keep the patient under a “wait and watch” policy. In such cases, the cancer may not be virulent and may not require any further treatment. | This kind of prostate cancer grows and spreads and it is important to treat rather than wait and watch. | The cancer is likely to grow and spread fast and may have already spread to other organs. The disease can be quite aggressive and further evaluation may be necessary to check on the spread of the cancer called metastasis. |
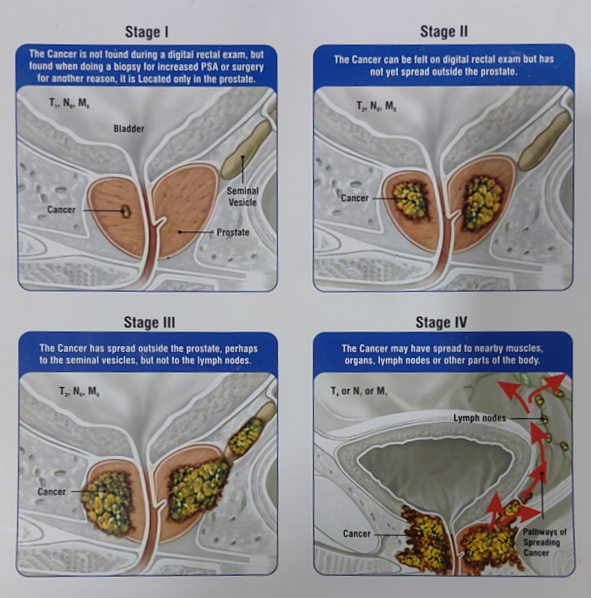
Stages Of Prostate cancer
The staging of prostate cancer depends on how far the cancer has spread; clinicians classify it as localized, locally spread, or distantly spread. The following diagram will aptly describe the staging of the prostate cancer.
- Stage I – Clinicians consider the cancer slow growing; they cannot feel the tumour during a digital rectal examination, and it involves one-half of one side of the prostate or less.
The cancer cells look similar to healthy cells, and the PSA levels are low. - Stage II – Clinicians find the cancer only in the prostate and can feel it during a digital rectal examination. Although the tumour remains small, it carries a higher risk of growing or spreading to other areas of the body.
PSA levels are low or medium.
- Stage III – High PSA levels, evidence that the tumor has grown beyond the prostate—possibly into the seminal vesicles but not the lymph nodes—or a high-grade classification indicate more advanced disease.
- All of these factors may indicate that the cancer could grow and spread.
- Stage IV – The cancer has spread beyond the prostate to other areas of the body to the nearby muscles & lymph nodes.
Treatments Of Prostate cancer
Various treatment options are employed:
- Active Surveillance
- Radical Surgery
- Radiation therapy
- Hormonal therapy
- Chemotherapy
Active Surveillance
Clinicians recommend active surveillance when prostate cancer is small and low grade. During surveillance, they monitor the patient with repeat PSA tests at variable intervals along with DRE examinations. In some cases, they also require a repeat biopsy.
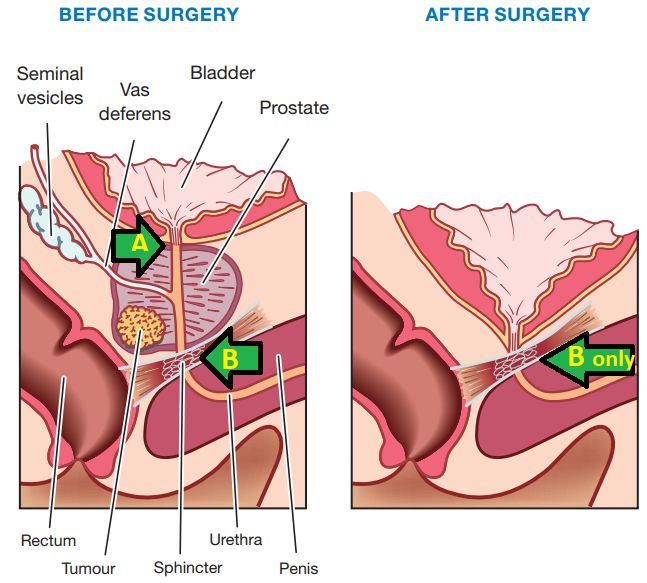
Radical Prostatectomy
Radical prostatectomy involves surgically removing the prostate gland to eliminate prostate cancer growth, along with the seminal vesicles. Surgeons perform this procedure when the cancer remains confined to the prostate gland and a part of the urethra, without spreading outside the gland. If required, the surgeon also removes nearby pelvic lymph nodes through a pelvic lymphadenectomy.
This can be achieved by :
- Open Radical Prostatectomy
- Laparoscopic Radical Prostatectomy or
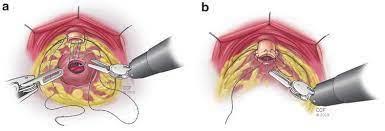
- Robotic Radical assisted Prostatectomy (RARP)
Radiation Therapy – External beam
This therapy gives radiation to the localized area to kill the prostate cancer cells. Clinicians generally undertake this when surgery is too risky due to medical conditions such as a history of cerebral stroke, coronary bypass (CABG), poor overall health, or other contraindications. In addition, radiation therapy typically requires more than 30–35 sessions and extends over a period of three months. They also use this approach as primary therapy in selected cases.
Radiation therapy – Brachytherapy
Low-dose seed implant brachytherapy
Clinicians insert seeds through the skin in the perineum (the area between the anus and scrotum). They perform the procedure under either general or spinal anaesthesia, and it takes approximately one hour.
High Dose Brachytherapy (HDR)
Under anaesthesia, clinicians insert approximately 15 needles through the perineum. They wire these needles to a radiation source, which delivers a high dose of radiation to the prostate. They then remove the needles.. The treatment takes 10–20 minutes.
Treatments Of Advance Prostate cancer
- Hormone therapy
when prostate cancer spreads outside the prostate gland or recurs after previous treatments, and they perform it through either medical or surgical orchidectomy.
- Bilateral Subcapsular Orchidectomy
In bilateral subcapsular orchidectomy, surgeons remove the substance of the testicles, which stimulates the growth of prostate cancer cells. They call this procedure surgical orchidectomy. However, when surgery is contraindicated, they use medical orchidectomy instead.
- Chemotherapy
Use specific anti-cancer drugs in advanced, metastatic, or recurrent cancer when hormone therapy has also failed.
Advanced Prostate Cancer Treatment Options
Treatment depends on the stage and severity of the cancer :
Active surveillance
For slow-growing cancer, regular monitoring without immediate treatment.
Medications & hormone therapy
Helps slow or stops cancer growth.
Minimally Invasive Therapy
Advanced surgical techniques ensure faster recovery and less discomfort.
Radiation Therapy
Targets and destroy cancer cells effectively.
Treatment is personalized based on patient condition and health.
Follow-Up Treatments
- Patient should discuss follow-up care with your uro-surgeon.
- Every treatment of prostate cancer may have some side effects and complications related to the treatment options. This needs to be understood and accordingly counselling and /or prevention therapy will be advised by Uro-Oncologist Dr. Dilip Raja, recognized as the best prostrate cancer doctor in Mumbai.
- Good nutrition is discussed after successful completion of treatment.
Preventions
- Some risk factors—such as race, family history, and age—remain unchangeable; however, people can control other factors, especially diet and weight. In addition, the Prostate Cancer Foundation suggests that men who want to reduce their risk of prostate cancer should make appropriate lifestyle changes.
- Eat fewer red meats and high-fat dairy products
- Good Nutrition – to be discussed after completion of successful treatment.
- Eat five or more servings of vegetables and fruits each day,
- Exercise regularly and
- Maintain a normal weight.

