NOW AVAILABLE AT BREACH CANDY HOSPITAL ON THURSDAYS 11:00 AM TILL 12:00 PM

Dr. Dilip Raja
Urologist & Andrologist
Urinary Incontinence
More common in females than in males
Get in touch with us today (+91 9820074649 )
Urinary Incontinence
- The experience of uncontrollably leaking urine can be an embarrassing issue for many people.
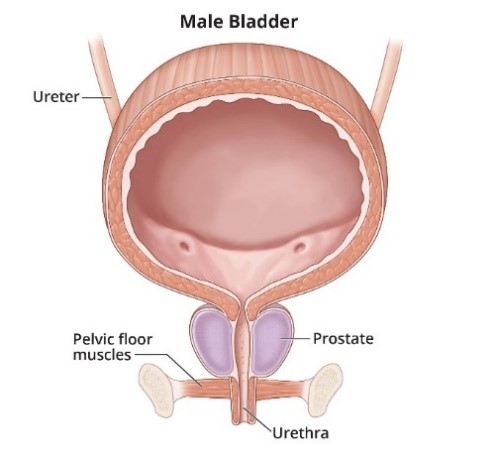
- Urinary incontinence is a loss of bladder control that’s commonly seen in older adults and women who have given birth or gone through menopause. Urinary tract infections (UTIs), pelvic floor disorders and an enlarged prostate are other causes.
- Urinary incontinence is when a person cannot prevent urine from leaking out.
- It can be due to stress factors, such as coughing, it can happen during and after pregnancy, and it is more common with conditions such as obesity.
- The chances of it happening increase with age.
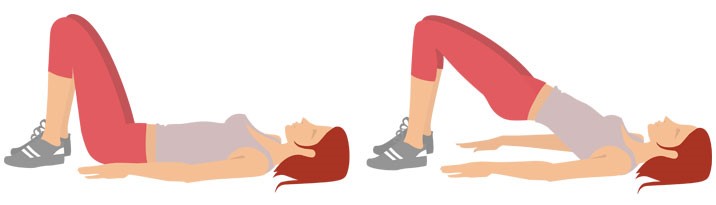
- Bladder control and pelvic floor, or Kegel, exercises can help prevent or reduce it.
Fast Facts On Urinary Incontinence
- Urinary incontinence is more common in females than in males.
- There are a number of reasons why urinary incontinence can occur.
- Obesity and smoking are both risk factors for urinary incontinence.
Types of Urinary Incontinence
There are several different types of incontinence. These types have different causes, characteristics and triggers for urine leakage. Knowing the type of incontinence is often an important part of the diagnosis and treatment plan for incontinence.

- Urge incontinence: This type of incontinence is characterized by an intense need to urinate right away. Often, this happens too quickly for you to make it to a toilet and you end up leaking urine. Urge incontinence can be caused by a condition called overactive bladder (OAB). You could have OAB for a variety of reasons like having weak pelvic muscles, nerve damage, an infection, low levels of estrogen after menopause or a heavier body weight. Some medications and beverages like alcohol and caffeine can also cause OAB.
- Causes: The following causes of urge incontinence have been identified:
- cystitis, an inflammation of the lining of the bladder
- neurological conditions, such as multiple sclerosis (MS), stroke, and Parkinson’s disease
- enlarged prostate, which can cause the bladder to drop, and the urethra to become irritated
- Causes: The following causes of urge incontinence have been identified:
- Stress incontinence: When you leak urine during activities, this is often stress incontinence. In this type of incontinence, your pelvic floor muscles are weak and no longer support your pelvic organs as they should. This muscle weakness means that you’re more likely to accidently leak urine when you move around. For many people, leakage issues happen when they laugh, cough, sneeze, run, jump or lift things.These actions all place pressure on your bladder. Without the support of strong pelvic muscles, you’re more likely to leak urine. Women who have given birth are at a higher risk of having stress incontinence. Men who have had prostate surgery may develop stress incontinence.
- Causes:
- pregnancy and childbirth
- menopause, as falling estrogen can make the muscles weaker
- hysterectomy and some other surgical procedures
- age
- obesity
- Causes:
- Overflow incontinence: If your bladder doesn’t empty completely each time you urinate, you could have overflow incontinence. Think of the bladder as a juice jug. If you only pour some of the juice out of the jug, but not all of it, there’s still a risk that you could spill when you move around. People with overflow incontinence never completely empty the bladder — placing them at risk for a spill. Usually, this results in small amounts of urine dripping out over time instead of one big gush of urine.This type of incontinence is more common in people with chronic conditions like multiple sclerosis (MS), stroke or diabetes. This may also occur in men with a large prostate.
- Causes:
- an enlarged prostate gland
- a tumour pressing against the bladder
- urinary stones
- constipation
- urinary incontinence surgery which went too far
- Causes:
- Mixed incontinence: This type of incontinence is a combination of several problems that all lead to leakage issues. When you have mixed incontinence, you might be dealing with stress incontinence and an overactive bladder. It’s often important to pay attention to what you’re doing when you have leakage issues with this type of incontinence. Identifying what triggers mixed incontinence is usually the best way to manage it.
- Causes:
- an anatomical defect present from birth
- a spinal cord injury that impairs the nerve signals between the brain and the bladder
- a fistula, when a tube or channel develops between the bladder and a nearby area, usually the vagina
- Causes:
- Other Causes:
- some medications, especially some diuretics, antihypertensive drugs, sleeping tablets, sedatives, and muscle relaxants
- alcohol
- Urinary Tract Infection (UTIs)
Diagnosis of Urinary Incontinence
- A bladder diary: The person records how much they drink, when urination occurs, how much urine is produced, and the number of episodes of incontinence.
- Physical exam: The doctor may examine the vagina and check the strength of the pelvic floor muscles. They may examine the rectum of a male patient, to determine whether the prostate gland is enlarged.
- Urinalysis: Tests are carried out for signs of infection and abnormalities.
- Blood test: This can assess kidney function.
- Postvoid residual (PVR) measurement: This assesses how much urine is left in the bladder after urinating.
- Pelvic ultrasound: Provides an image and may help detect any abnormalities.
- Stress test: The patient will be asked to apply sudden pressure while the doctor looks out for loss of urine.
- Urodynamic testing: This determines how much pressure the bladder and urinary sphincter muscle can withstand.
- Cystogram: An X-ray procedure provide an image of the bladder.
- Cystoscopy: A thin tube with a lens at the end is inserted into the urethra. The doctor can view any abnormalities in the urinary tract.
Treatment Of Urinary Incontinenece
Treatment will differ depending on the type of incontinence, age, level of health and mental state of the patient.
- Lifestyle changes: For stress incontinence, Kegel exercises could help strengthen your pelvic floor muscles which help control urination. To control the urge to urinate, you can also train your bladder by delaying urination, controlling your urination by starting, stopping, and then going to urinate again (called double voiding), and having a bathroom schedule, such as going to urinate every 2 hours or so.
- Medication: Medication such as anticholinergics or beta-agonists may also be prescribed to calm overactive bladders. Topical oestrogen could also strengthen the tissues in the urethra and vaginal areas to alleviate symptoms.
- Surgery: Surgical options include the sling procedure (mesh inserted under the neck of the bladder to support the urethra), colposuspension (lifting the bladder neck and relieve stress incontinence) and implanting an artificial sphincter (inserted to control the flow of urine from the bladder into the urethra).
